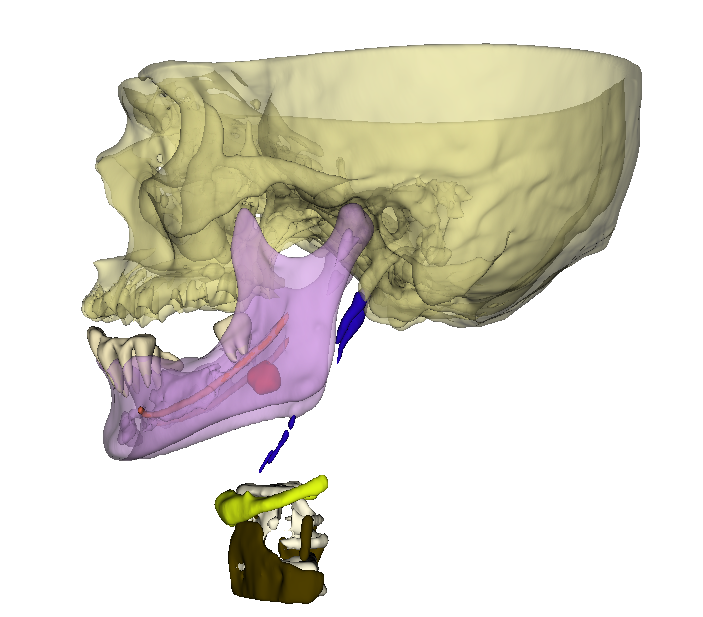
What Is Partial Volume Averaging?
Imagine a digital image, where each point (pixel) is a mix of the colors it “sees.” Now, in 3D medical scans like CBCT, each “box” in the scan (called a voxel) collects information from the tissue it covers. If that box only contains bone, it will show up as bone in the scan. But if it straddles both bone and soft tissue, the scan averages these materials together. The voxel doesn’t know which is which — so the final image shows a gray area, a mix between bone and tissue.
This mixing is called partial volume averaging. It’s like looking at a patchwork quilt through frosted glass: the fine details blend, and crisp boundaries fade.
The effect is strongest when the objects being scanned are smaller than, or similar in size to, the voxels used in the scan.
How Partial Volume Averaging Occurs in CBCT
- In CBCT, larger voxel sizes or lower scan resolutions increase the risk of this artifact—small anatomical structures or thin layers appear blurred or misrepresented because the signal within a voxel represents a mix of materials.
- Studies comparing CBCT to micro-CT (the gold standard for fine detail) have specifically identified partial volume effects responsible for underestimation or overestimation of actual structural volumes in teeth, bones, and other features.
- This effect is not unique to conventional CT; any 3D imaging modality that averages X-ray data into voxels, including CBCT, is susceptible.
Partial volume averaging has a significant effect on segmentation models in CBCT, especially those based on AI and deep learning. Because partial volume averaging causes voxels to contain mixed tissue types leading to blurred or averaged intensities, it complicates accurate boundary detection and tissue classification in segmentation tasks.
Effects on CBCT Segmentation Models & Implant Planning
Do you know PVA can effect segmentation protocols. The impact of partial volume averaging can be quite large, especially for clinical applications requiring high precision such as surgical guides or implant planning where millimeter accuracy is critical. Studies demonstrate that partial volume effects can cause segmentation deviations up to several millimeters, which may adversely impact treatment decisions.
- Blurring of Boundaries: Partial volume effect causes unclear or fuzzy edges between different anatomical structures, making it hard for segmentation models to precisely delineate boundaries such as the mandibular canal, thin bone, or pulp chambers.
- Undersegmentation: Important small structures or delicate features can be missed by AI models because the partial volume effect reduces signal contrast, leading to undersegmentation or incomplete segmentation.
- Volume Measurement Errors: Due to voxel averaging, segmented volumes may be underestimated or overestimated, affecting any quantitative analysis or 3D modeling derived from the segmentation.
- Reduced Model Accuracy: Segmentation accuracy decreases particularly in areas where anatomical complexity is high or structures are near the voxel size resolution limit.
How did the contemporary AI segmentation algorithms manage this PVA artefact?
- Many modern AI segmentation models incorporate partial volume effect modeling or estimation within their algorithms, improving their ability to handle mixed voxels by predicting tissue proportions inside each voxel rather than binary classification.
- Training on large, diverse CBCT datasets with varying resolutions helps models generalize better and reduce errors caused by partial volume effects.
- Some segmentation workflows include post-processing corrections or manual refinements to overcome undersegmentation caused by partial volume averaging.
Where Do Partial Volume Artifacts Emerge in CBCT?
Dental Roots and Periodontal Ligament: When thin layers like the periodontal ligament or root fractures are smaller than the voxel size, they may disappear or appear thicker/thinner than reality.

Sinus Walls and Nasal Structures: Thin bone plates of the sinus or nasal walls can blend into the adjacent air, blurring critical margins.
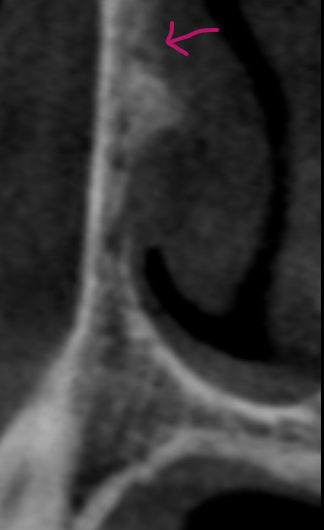
Jawbone and Alveolar Ridge: Narrow bony ridges or defects from resorption may not be clearly visualized, making measurement uncertain.
Airway Assessment: In airway or sinus imaging, small walls (like septa) may appear thicker, and airway diameters could be underestimated or blurred.
Pulp Chambers or Canals: Narrow pulp spaces inside teeth may appear larger or might be missed, especially in young patients or in teeth with fine canal anatomy.

Implant Sites: Assessment of very fine bone around potential implant sites can be compromised, hiding defects or exaggerating bone thickness.
Thin cortical bone plates: Such as the walls of the maxillary sinus, nasal cavity, and around the alveolar ridge, where the thin bone boundaries can be blurred.
Trabecular bone: The fine meshwork of trabecular bone is often over- or underestimated due to voxel averaging in CBCT.
Air cavities: Interfaces between air (high contrast) and soft tissue or bone, like in sinus or airway imaging, where partial volume can cause boundary blurring.
TMJ joint spaces and condylar bone: Due to the small size and complex morphology of the temporomandibular joint.

Thin cartilage and soft tissue layers adjacent to bone: Because CBCT has limited soft tissue contrast, partial volume effects can further obscure soft tissue boundaries.
These regions are especially sensitive because the voxel may contain a mix of bone, soft tissue, and air, causing the signal within that voxel to be an average and thus reducing image sharpness and accuracy.
Why Does This Matter for TMJ Scans in CBCT?
The temporomandibular joint (TMJ) is a complex, small joint where your jaw connects to your skull. Problems here can be subtle and detailed. CBCT is widely used for TMJ imaging, offering 3D views with far less radiation than traditional CT.
However, the main challenge is that the bony parts of the joint — like the condylar head and the thin bone of the glenoid fossa — often have fine features smaller than a typical CBCT voxel.

When the scan resolution isn’t high enough (that is, when voxels are too big):
- Small holes or bone erosions may be hidden or smoothed out, making early disease hard to spot.
- Joint surfaces can look thicker, rounder, or flatter than they really are.
- Measurements of bone thickness or joint space may be inaccurate.
- Minor TMJ changes from arthritis, trauma, or developmental issues could be missed or misrepresented.
This is especially important for TMJ problems because many joint conditions begin with tiny changes in bone that are difficult to see unless the scan has very small voxels.
How to Overcome Partial Volume Averaging in CBCT
Use Smaller Voxel Size: Selecting the smallest available voxel size (thin slices) improves resolution, minimizing averaging and preserving detail, though at the expense of increased noise and possibly higher radiation.
Reduce Field of View (FOV): Targeting only the anatomical area of interest increases resolution for that region and reduces artifact occurrence.
Optimal Slice Orientation & Thickness: Aligning slices with the structure of interest lessens the chance of averaging across different tissue types. At the same time reduce the slice thickness so that all the averaging structures are removed.
Careful Patient Positioning: Ensuring the structure of interest is in the center of the FOV reduces peripheral artifacts.
Expert Image Interpretation: Radiologists/dentists must be aware of locations prone to this artifact, so they don’t misdiagnose or mis-measure.
Post-processing Corrections: Some advanced algorithms and image processing tools can help estimate and compensate for partial volume errors after scanning, though these are less widely available.
Repeat Scans if Indicated: In rare cases where tiny details are essential, and artifact obscures findings, rescanning with optimized settings may be necessary.
Conclusion
Partial volume averaging is a blending effect in 3D CBCT scans, caused when a voxel contains more than one type of tissue. For CBCT TMJ scans, this can hide or blur important bone changes.
Choosing high-resolution scan settings, focusing only on the TMJ, and expert interpretation are key to reducing this artifact and making sure vital TMJ problems aren’t missed.
- Steiner’s Analysis – Free online Cephalometry - November 23, 2025
- A Complete guide to Grayscale values in CT & CBCT - November 15, 2025
- Struggling to get your old PC to run new Radiology software smoothly? Here’s a trick with SSD that might save you. - November 14, 2025